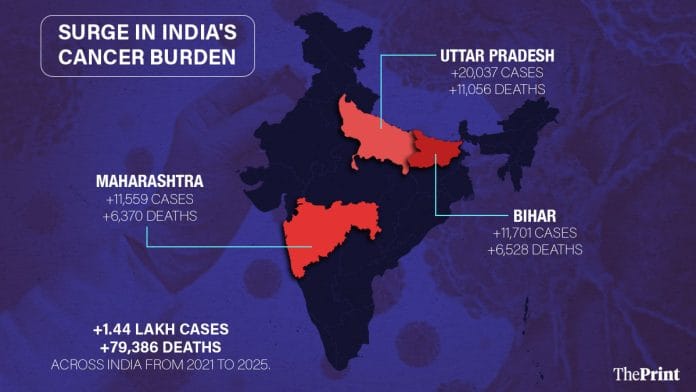
The figures were shared by Minister of State for Health Prataprao Jadhav Tuesday, in response to a question in the Rajya Sabha. Estimates are from the Indian Council of Medical Research (ICMR)-National Cancer Registry Programme (NCRP).
Large and populous states have seen the biggest increase in cancer cases.
Uttar Pradesh recorded the sharpest rise, with estimated cases up from 2,06,088 in 2021 to 2,26,125 in 2025—a rise of more than 20,000 cases. Bihar and Maharashtra followed close behind, each registering more than 11,000 additional cases in the same period.
Mortality has also risen significantly in these states. Uttar Pradesh recorded the largest overall rise in cancer deaths in India—an increase of more than 11,000 between 2021 and 2025. In Bihar, cancer deaths increased by 6,528 while Maharashtra saw an additional 6,370 deaths over the five-year period.

According to Dr Mukurdipi Ray, surgical oncologist at New Delhi’s All India Institute of Medical Sciences (AIIMS), the rise is consistent with projections from the NCRP.
“This trend reflects a steady crude annual increase, largely driven by population growth and an aging demographic profile. Although the nearly 10 percent rise over five years—averaging around 28,000 additional cases annually—is substantial in absolute terms for an already resource-constrained healthcare system, the increase remains relatively modest on a per capita basis, with the crude incidence rate still around 100 per 100,000 population,” Dr Ray told ThePrint.
A part of this rise may also reflect improved diagnostic reach and better cancer registration rather than a dramatic surge in true biological incidence, Dr Ray added.
The surge in cases is significant from a public health perspective.
Dr Ray explained that it imposes a growing burden on densely populated states such as Uttar Pradesh, Bihar, and Maharashtra, where case load is particularly high.
“While age-adjusted incidence rates remain relatively stable in some registry-based analyses, persistent underreporting in rural and underserved regions suggests that the actual burden may be considerably higher than current estimates indicate,” he said.
Multiple factors are contributing to this upward trend. While expanded diagnostic facilities, improved imaging, and broader registry coverage may account for a significant share of the estimated increase, Dr Ray said that genuine epidemiological drivers are also at work.
“(These include) Rising life expectancy, tobacco use, unhealthy dietary habits, physical inactivity, obesity and environmental exposures. Air pollution in metropolitan areas and water contamination in vulnerable regions may further aggravate cancer risk, particularly in high-population northern states.”
According to the health ministry, research has linked certain environmental factors with cancer risk. A 2025 review cited by the government noted that contamination of water sources by industrial waste, pesticides, heavy metals and pharmaceutical pollutants may be associated with rectal and colorectal cancer.
To tackle the growing burden, the government says it is expanding cancer care infrastructure across the country.
Under the Strengthening of Tertiary Care Cancer Facilities Scheme, 19 state cancer institutes and 20 tertiary care cancer centres have been approved to improve access to treatment, the ministry said.
In addition, Tata Memorial Centre in Mumbai has set up hospitals in cities such as Varanasi, Visakhapatnam, New Chandigarh, Guwahati, Sangrur and Muzaffarpur to provide specialised cancer care.
Cancer treatment facilities have also been approved in all 22 new AIIMS, while institutions such as the National Cancer Institute in Jhajjar and the second campus of the Chittaranjan National Cancer Institute in Kolkata are designed for diagnosis, research and treatment.
In the Union Budget 2025-26, Finance Minister Nirmala Sitharaman had announced setting up of Day Care Cancer Centres in all district hospitals over the next three years. The government had approved 297 centres for 2025-26. These centres aim to allow easier access to chemotherapy and reduce the burden on tertiary hospitals.
Meanwhile, schemes such as Ayushman Bharat-Pradhan Mantri Jan Arogya Yojana (PM-JAY) provide health insurance coverage of up to Rs 5 lakh per family per year for hospitalisation, including cancer treatment, at empanelled hospitals.
“Government initiatives represent important progress in expanding access to cancer treatment. However, major gaps remain. India continues to face a shortage of trained oncologists, limited radiotherapy infrastructure and late-stage diagnosis, with nearly 60-70 percent of patients still detected at advanced stages,” Dr Ray said.
He added that population-based screening for breast, cervical and oral cancers needs to be intensified, particularly in high-burden states such as Uttar Pradesh, Bihar and Maharashtra.
“Expanding HPV vaccination, strengthening tobacco cessation programmes and improving early referral through frontline health workers can significantly improve early detection and outcomes,” said the doctor.
(Edited by Nida Fatima Siddiqui)